Depression and inflammation often travel together in ways that can feel confusing, even scary. You might tell yourself, “I’m just depressed,” but what you’re living with is also physical: the lead-weight fatigue, the body aches that make a quick walk to the subway feel like a marathon, the brain fog that turns simple emails into a mountain.
In our Midtown Manhattan psychiatry practice, we see this mind-body overlap every week, especially in New Yorkers juggling high-demand jobs, caregiving, chronic medical conditions, or all three at once. The good news is that when your symptoms are taken seriously as whole-person symptoms, not “all in your head,” treatment can become more precise, and often more hopeful.
Depression and Inflammation: why depression can feel so physical
If depression were only an emotion, it would be easier to “talk yourself out of.” Many patients try, and then feel ashamed when it doesn’t work. But depression can change how your body runs, how you sleep, how you move through the day, and how much effort everything takes.
The symptoms patients describe
People rarely walk into an appointment and say, “Hello, I have depression.” More often, they say:
- “I’m exhausted all the time, even after sleeping.”
- “My body hurts, and my labs are ‘fine.’”
- “I can’t think clearly. I keep rereading the same paragraph.”
- “My sleep is broken, and then my mood crashes.”
- “Nothing feels rewarding, even when life looks good on paper.”
Those experiences are real. They can be consistent with depression, and they can also overlap with medical conditions, chronic stress, grief, hormonal shifts (including postpartum or perimenopause), and medication side effects. That overlap is one reason a careful, individualized evaluation matters.
A simple analogy: the body’s smoke alarm is stuck on
Inflammation is part of the immune system’s normal job. It is how your body responds to injury or infection. The problem is when the alarm keeps ringing even when there is no active fire.
When inflammation stays “on” in a low-grade, chronic way, some people feel it as:
- heavy fatigue
- increased pain sensitivity
- slowed thinking and motivation
- sleep disruption
This is one way depression and inflammation can reinforce each other, and why depression can feel pervasive, not just emotional.
What research suggests about Depression and Inflammation, and what it does not
Researchers have been studying depression and inflammation for years, and the overall message is nuanced.
What we know so far
Studies have found that some people with depression show signs of increased inflammation in the body, for example, higher levels of inflammatory markers on blood tests (a common one is CRP, a marker many primary care doctors already use to assess inflammation and cardiovascular risk). Researchers also study immune signaling chemicals (cytokines) because they can influence sleep, appetite, energy, and mood.
This does not mean depression is “just inflammation,” or that everyone with depression has an inflammatory profile. It means there may be subtypes of depression, and one subtype may be more inflammation-linked than another.
For background reading from trusted sources, see the National Institute of Mental Health overview of depression and clinical reviews indexed through the National Library of Medicine (search terms: “inflammation depression CRP cytokines”).
What this does not mean
It does not mean:
- You can diagnose depression with a single blood test
- Inflammation “causes” depression in every case
- You should self-treat with supplements or anti-inflammatory medications without medical guidance
Depression is multifactorial. Biology, psychology, sleep, relationships, trauma history, medications, substance use, and medical illness can all matter. The value of the inflammation lens is that it can reduce stigma and expand options, not replace the basics of good psychiatric care.
Depression and Inflammation in chronic medical illness: why the overlap is so common
If you are managing a medical condition, and depression shows up alongside it, many people immediately blame themselves: “I should be stronger.” From a clinical perspective, the overlap is common and meaningful.
Shared pathways can include immune activation, hormonal stress responses, and disrupted sleep and circadian rhythms. And then there is the human part: living with symptoms, uncertainty, and appointments can wear people down.
Cardiovascular disease
Depression is associated with worse outcomes in heart disease, in part because depression can drain motivation for self-care and make it harder to follow treatment plans consistently.
The American Heart Association summarizes the two-way relationship in patient-friendly terms, including why screening and treatment matter.
Diabetes
Diabetes management asks for steady routines, meals, medication timing, glucose monitoring, and follow-up visits. Depression can flatten the very skills you need to do those things.
At the same time, blood sugar swings can affect energy and mood, creating a feedback loop. The American Diabetes Association discusses how mental health and diabetes interact, and why integrated care helps.
Autoimmune disorders and chronic pain
Autoimmune conditions and chronic pain can overlap with depression through fatigue, sleep disruption, and nervous system sensitivity. Many patients describe feeling dismissed, or like they have to “prove” they are unwell. When depression and inflammation are both in the picture, a validating, coordinated treatment plan can be a turning point.
How Depression and Inflammation can look in daily life, especially in NYC
A Midtown executive may still be getting to meetings on time, but inside, everything takes twice the effort. A college student may think they have “attention problems” when the real issue is depression with cognitive slowing. A postpartum parent may feel terrified that the fog and numbness mean they are failing, rather than recognizing a treatable condition.
Here are a few patterns we hear often:
The “brain fog” pattern
You might notice:
- slower recall of words or names
- rereading without comprehension
- difficulty initiating tasks
- feeling mentally “cottony” by afternoon
This can be depression, sleep deprivation, anxiety, ADHD, medication effects, medical illness, or a combination. If cognition is a major complaint, it may be helpful to consider a more structured assessment, not to label you, but to clarify what is driving what.
If you want to understand what a formal cognitive workup involves, our guide to neuropsychological testing explains who it helps and what to expect.
The sleep disruption pattern
When sleep breaks down, mood regulation becomes harder for almost anyone. Some people with depression and inflammation describe waking up feeling like they never truly rested.
We have also written about sleep as a meaningful treatment target in its own right. Can sleep heal more than we think? for a practical overview, including evidence-based therapy options like CBT-I.
The “I’m functioning, but I’m not living” pattern
This is common among high-achieving New Yorkers. You may be meeting obligations while feeling emotionally flat, physically depleted, and privately frightened that you are “becoming a different person.” This is often the moment when patients benefit from a comprehensive plan rather than piecemeal advice.
Treatment: a comprehensive approach that respects both mind and body
When patients hear “mind-body connection,” they sometimes worry the clinician is about to minimize their physical symptoms. The opposite is true. A whole-person approach is a way to take physical symptoms seriously while still treating mood effectively.
Start with a real evaluation, not just a questionnaire
Online screeners can be useful, but they are not a diagnosis. A thorough psychiatric evaluation explores symptom history, medical factors, medications, sleep, stressors, and risk, then maps treatment to your specific pattern.
If you are deciding what type of assessment you need, our article on psychiatric evaluation vs online mental health questionnaires breaks down the differences.
Psychotherapy that targets the way depression runs your day
For depression and inflammation presentations, therapy is not about “positive thinking.” It is about helping you regain traction, especially when motivation and energy are low.
At Dr. Iospa Psychiatry Consulting PC, psychotherapy may include CBT, DBT, or supportive therapy depending on your needs and the story behind your symptoms. The goal is practical: reduce suffering, improve functioning, and help you feel like yourself again.
Medication management, when indicated, with careful monitoring
Some patients benefit from medication, particularly when symptoms are persistent, severe, or biologically “sticky.” Medication can improve sleep, energy, concentration, and the ability to engage in therapy.
If you are curious about how psychiatrists think about depression treatment options, you may find this helpful: The role of psychiatrists in treating depression.
If you have tried treatment before and felt discouraged, our post on why depression treatment fails for some patients may help normalize what is often just a sign that the plan needs to be more personalized.
Cognitive support when thinking and focus are part of the problem
When depression shows up with cognitive slowing, attention problems, or post-illness brain fog, targeted cognitive work can be valuable. In our practice, this may include Cognitive Remediation Therapy (CRT) when appropriate.
YouTube integration suggestion (for your editor): consider embedding a short segment from our CRT video series within this section to help readers understand what CRT looks like in real life. Related internal page: Cognitive Remediation 3-Part Series.
Clinical investigations: where GLP-1 fits, and where it does not
You may have seen headlines about GLP-1 medications (often prescribed for diabetes and weight management) and mental health. Researchers are actively studying whether GLP-1 receptor agonists may influence inflammation and brain pathways that could be relevant to mood in some patients.
At this time, GLP-1 medications are not established or universally accepted treatments for depression, and they are not a substitute for evidence-based depression care. If you are already taking a GLP-1 for a medical condition and you notice mood changes (better or worse), that is worth discussing with your prescribing clinician and your psychiatric provider so your care team can coordinate safely.
When to seek help, and what to expect in Midtown Manhattan or via telehealth
Consider reaching out for professional support if you notice:
- persistent low mood or loss of interest
- fatigue that does not improve with rest
- brain fog, slowed thinking, or trouble concentrating
- sleep or appetite changes that are sticking around
- physical symptoms (aches, heaviness) that track with mood
At Dr. Iospa Psychiatry Consulting PC, we provide comprehensive psychiatric and psychological services in Midtown Manhattan and via telepsychiatry across New York. Care may include psychiatric evaluation, psychotherapy, medication management, and, when appropriate, neuropsychological or psychoeducational testing.
Our team includes Alla Iospa, Konstantin Nikiforov, Yana Serobyan, and Elizabeth Zharovsky, working collaboratively so patients are not left to connect the dots alone.
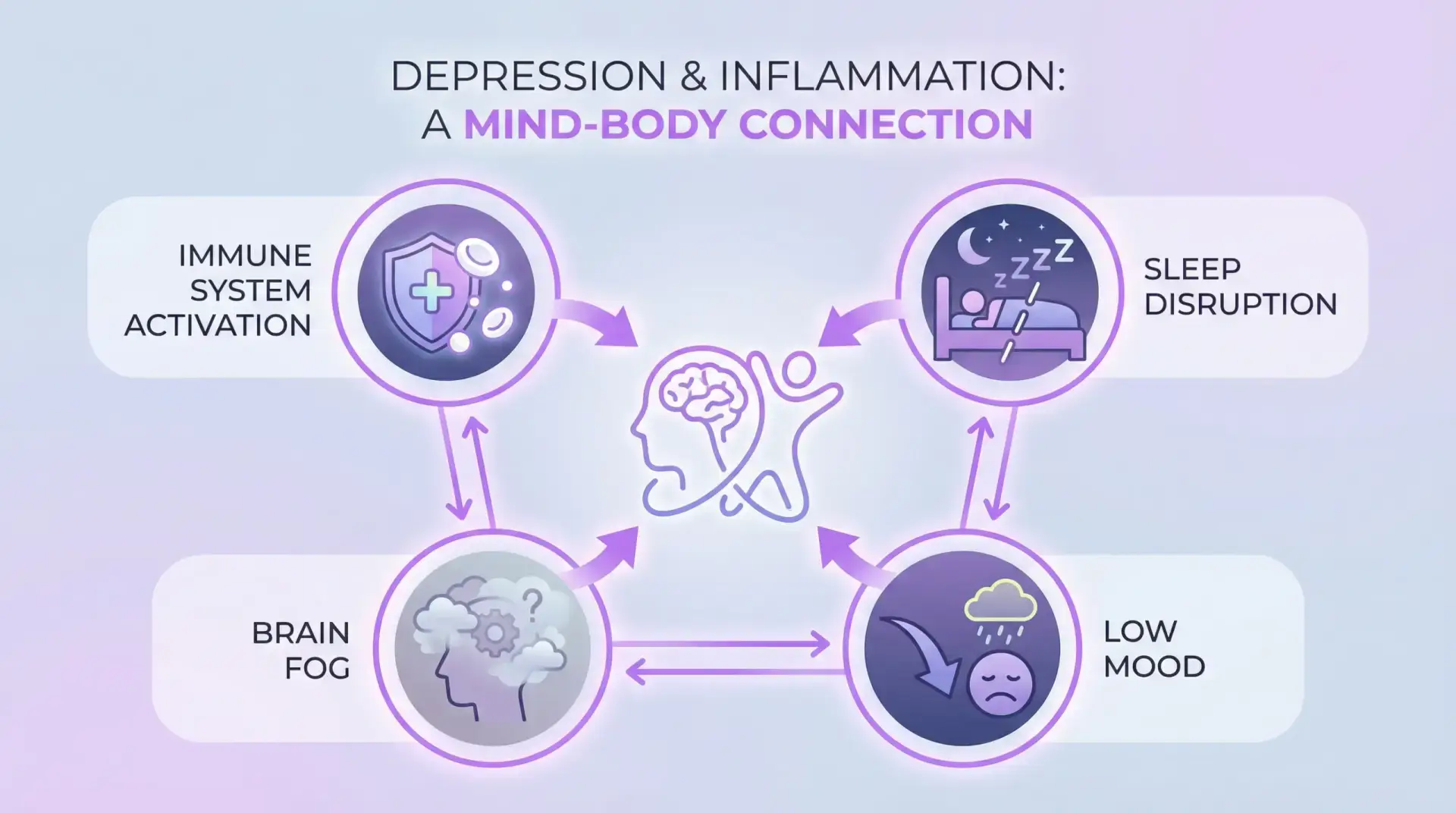
Caption: A simple way to visualize how depression and inflammation can interact through sleep, cognition, and energy.
Description: A clean, patient-friendly diagram showing four connected nodes: immune activation, sleep disruption, brain fog, and low mood, illustrating a feedback loop.
Frequently Asked Questions
Is depression really connected to inflammation? For some people, yes. Research suggests a subset of depression is associated with increased inflammatory activity, which may contribute to fatigue, pain sensitivity, and brain fog. It is not the only cause of depression, and it does not apply to everyone.
What are the signs that my depression is affecting my body? Many patients report low energy that feels physical, body aches, disrupted sleep, changes in appetite, and cognitive slowing. These symptoms are common in depression and also overlap with medical conditions, so evaluation matters.
Should I ask my doctor to check inflammatory markers? It depends on your history, symptoms, and medical risk factors. Some clinicians may check labs (often through primary care) to rule out medical contributors and assess inflammation. Your psychiatric provider can help coordinate what is appropriate.
If I have a chronic illness, is it “normal” to feel depressed? It is common, but you do not have to accept it as your new baseline. Chronic illness can increase depression risk through stress, sleep disruption, and inflammation pathways. Treatment can improve both quality of life and daily functioning.
Can therapy help if my depression feels biological? Yes. When depression and inflammation are in the picture, therapy can still be very effective, especially when it focuses on behavior, sleep, coping patterns, and self-criticism that intensify symptoms. If anxiety is part of your picture alongside depression, see also Anxiety and Inflammation, which covers similar ground for the anxiety side of this overlap.
When should I consider neuropsychological testing? If brain fog, memory concerns, or attention problems are central, testing can clarify whether symptoms fit depression, anxiety, ADHD, cognitive change, or a combination. It can also guide treatment and accommodations.
Ready for care that treats the whole picture?
If you are dealing with depression that shows up in your body, not just your thoughts, you deserve a plan that reflects that reality. Dr. Iospa Psychiatry Consulting PC offers comprehensive, personalized psychiatric and psychological care in Midtown Manhattan and online, including psychotherapy, medication management, and, when appropriate, neuropsychological evaluation.
Explore options for getting started at Dr. Iospa Psychiatry Consulting PC and consider reading Depression Treatment in Midtown NYC: How to Spot the Hidden Signs if you are unsure whether what you are feeling “counts.”
Educational disclaimer: This article is for educational purposes only and is not medical advice. If you are in crisis or thinking about self-harm, call or text 988 (Suicide & Crisis Lifeline) or go to the nearest emergency room.